End of the golden epoch of antibiotics
- Use of low dose antibiotics in agriculture
- Failure of completion of a full course of treatment
- Prescription of antibiotics for treating viral infections
with appropriate approach to cleaning and disinfection, we can save approximately 10.000.000 lives in 30 years, by preventing transmissions of MDR within hospital and healthcare facilities
can lead to fierce strains of bacteria that are resistant to more than one antibiotic. Sharing of genetic material between a resistant strain and a sensitive strain can lead to the spread of this resistance. When these multi-drug resistant (MDR) bacteria infect a person, the disease becomes aggressive and almost impossible to treat.
These ‘superbugs’ are more prevalent in hospitals because that is where most of the antibiotics are used.
Approximately two million people become infected with MDR bacteria in the US each year. 23000 die from these infections. By 2050, MDR bugs could kill around 10 million people annually. Journalist Maryn McKenna, in her recent TED talk discusses the dawn of the ‘post-antibiotic era’.
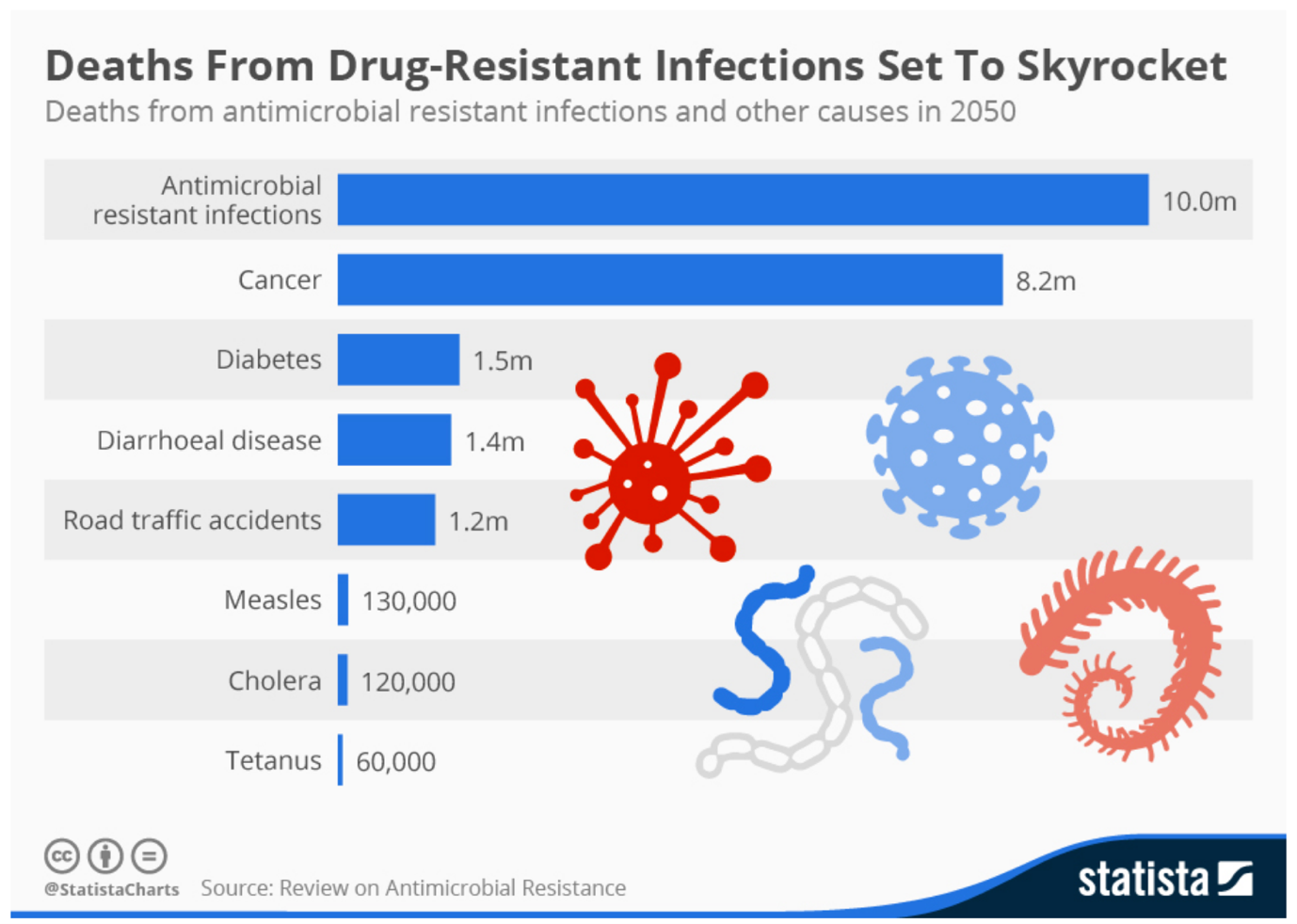
Number of people predicted to die of antibiotic-resistant infections by 2050
Therefore, it is necessary for hospitals and healthcare facilities to take measures for controlling the development of antibiotic resistance. Controlling is necessary in this case, since the cause of deaths associated with MDR (in next 30 years) will increase rapidly, and will overcome deaths associated with cancer for almost 20 % (19,78 %). That means that with appropriate approach to cleaning and disinfection, we can save approximately 10.000.000 lives in 30 years, by preventing transmissions of MDR within hospital and healthcare facilities.
Other than encouraging correct antibiotic usage, hospitals must pay attention to disinfection procedures and environmental cleaning protocols. Patient rooms, bathrooms, high-touch areas in out-patient departments as well as ICUs are hotbeds of residual bacteria. Unless these areas are thoroughly cleaned and disinfected regularly, we cannot slow down the antibiotic-resistance. UVC technology is the most intensely studied alternative to conventional disinfection procedures in hospitals. At 254nm UV-C radiations can damage DNA by inducing formation of pyrimidine dimers. DNA damage can reduce the replicative ability of microorganisms severely. Areas frequently missed by cleaning staff, such as edges of tables, corners and crevices remain contaminated. A UV-C lamp provides a uniform coverage for these problem areas. The inadequacy of standard manual decontamination procedures has spurred the development of automated environmental cleaning systems, such as SteriPro UV-C disinfection robot from Europe.

SteriPro robot disinfecting operating room
These devices report 6-7 Log reduction of the burden of bacteria in in-vitro experiments. SteriPro offers significant advantage over contactless disinfection procedures (fogging - aerosol of hydrogen peroxide) and requires ZERO operational supervision, and does not take a lot of time, to achieve optimal disinfection results, and only minimal preparation. Real-time reports and online monitoring of disinfection cycles allows easy incorporation of this technology in hospital’s established disinfection workflows and frees up time for personnel. Hospitals can decide on an appropriate UV-C device keeping in mind the room capacity, peak turnover times, usability and workflow assessments, and most importantly, patient and staff safety.



